Key Takeaways
- Pain at the base of the thumb is one of the most common hand complaints, affecting up to 33% of women and 11% of men over age 50.
- The three most likely causes are thumb arthritis (rhizarthrosis), de Quervain’s tenosynovitis, and tendinitis — each with distinct patterns.
- A simple self-assessment of where it hurts, what triggers it, and how long it lasts can help you and your doctor narrow down the cause.
- You should see a doctor if pain persists beyond 2-3 weeks, wakes you at night, or limits your ability to grip or pinch.
If you have noticed a deep, aching pain right where your thumb meets your wrist, you are not alone. This is one of the most common hand complaints that doctors see, and it can make simple tasks — opening a jar, turning a key, even holding a cup — surprisingly difficult. The good news is that understanding what is causing your pain is the first step toward getting the right treatment.
Where Exactly Does It Hurt?
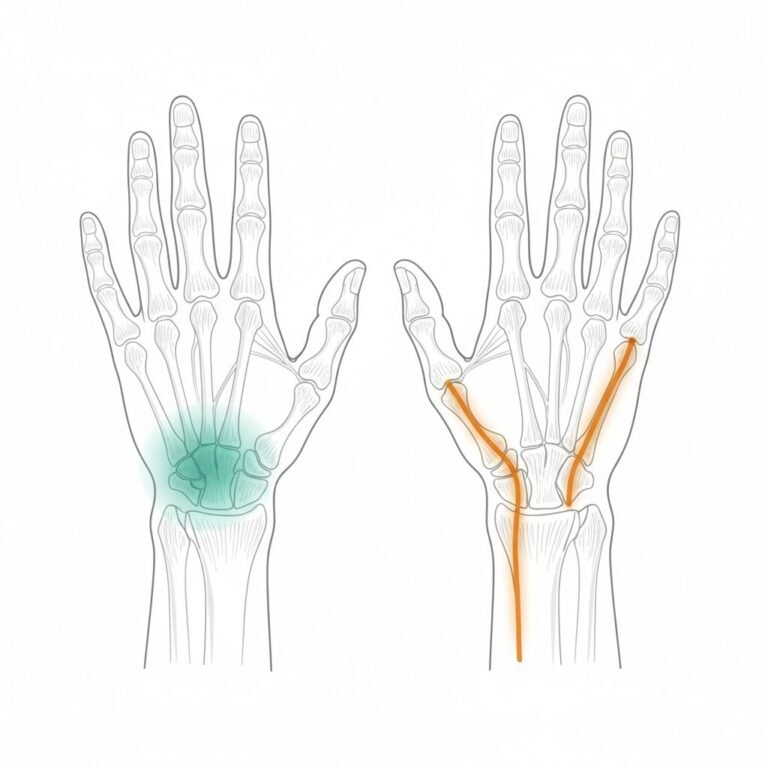
The base of your thumb is a busy intersection of bones, tendons, and ligaments. Pinpointing the exact location of your pain is one of the most helpful things you can do before your appointment. Here is a quick guide:
- Directly at the fleshy mound below your thumb (the thenar eminence): This often points to CMC joint arthritis (rhizarthrosis), where the thumb metacarpal bone meets the trapezium bone.
- On the wrist side, closer to the forearm tendons: This pattern is more common with de Quervain’s tenosynovitis, which involves inflamed tendons on the thumb side of the wrist.
- Along the thumb itself or at the knuckle: This may suggest trigger thumb, MCP joint arthritis, or a ligament injury.
The Three Most Common Causes
1. Thumb Arthritis (Rhizarthrosis)
Rhizarthrosis is osteoarthritis of the carpometacarpal (CMC) joint at the base of the thumb. It is the most common cause of persistent thumb base pain in adults over 40. The cartilage that cushions the joint gradually wears down, leading to bone-on-bone contact.
Typical signs:
- Deep aching at the thumb base that worsens with gripping, pinching, or twisting motions
- Stiffness first thing in the morning that lasts less than 30 minutes
- A grinding sensation when you move the thumb
- Swelling or a bony bump at the base of the thumb
- Reduced pinch and grip strength over time
- Pain that comes and goes at first but gradually becomes more constant
Research shows that rhizarthrosis is significantly more common in women, with prevalence rates of 25-33% in postmenopausal women compared to about 8-11% in men of the same age. Genetics, joint laxity, and hormonal changes all play a role. Learn more in our guide on who gets rhizarthrosis and why.
2. De Quervain’s Tenosynovitis
De Quervain’s involves inflammation of the tendons that run along the thumb side of the wrist (the abductor pollicis longus and extensor pollicis brevis). It is especially common in new parents, people who do repetitive hand movements, and women aged 30-50.
Typical signs:
- Sharp or burning pain on the thumb side of the wrist, not deep in the joint
- Pain when you make a fist, grasp objects, or turn the wrist
- Swelling over the wrist tendons, sometimes with a squeaky feeling
- A positive Finkelstein test (pain when you tuck the thumb inside a closed fist and bend the wrist toward your little finger)
For a detailed comparison, see our article on rhizarthrosis vs de Quervain’s.
3. Tendinitis and Overuse Injuries
General tendinitis at the thumb base can occur from repetitive activities — texting, gaming, gardening, or manual work. Unlike arthritis, tendinitis often improves significantly with rest within a few weeks.
Typical signs:
- Pain that started suddenly after a new or repetitive activity
- Tenderness along a specific tendon rather than deep in the joint
- Improvement with rest and worsening with the triggering activity
- No grinding sensation or bony changes
Self-Assessment: Questions to Ask Yourself
Before your appointment, consider these questions. Your answers will help your doctor make a faster, more accurate diagnosis:
- When did the pain start? Gradual onset over months suggests arthritis. Sudden onset suggests injury or tendinitis.
- What makes it worse? Pinching and gripping point to CMC arthritis. Wrist turning points to de Quervain’s.
- Is there morning stiffness? Arthritis typically causes stiffness lasting up to 30 minutes. Longer stiffness may suggest inflammatory arthritis.
- Do you feel grinding? A gritty or crunching sensation (crepitus) is a hallmark of joint arthritis.
- Has the shape of your thumb changed? A bony bump or a squared-off appearance at the base is common in moderate to advanced rhizarthrosis.
- Does rest help? Tendinitis usually improves with rest. Arthritis may feel better temporarily but returns with activity.
Red Flags: When to See a Doctor Soon
While most thumb base pain is not an emergency, certain signs mean you should seek medical attention sooner rather than later:
- Pain lasting more than 2-3 weeks that does not improve with rest and over-the-counter medication
- Night pain that wakes you from sleep
- Significant swelling, redness, or warmth at the joint — this could indicate infection or inflammatory arthritis
- Inability to grip or pinch that interferes with daily tasks like dressing, eating, or working
- Numbness or tingling in the thumb or fingers — this may suggest nerve involvement
- Pain after an injury such as a fall, which could mean a fracture or ligament tear
- Fever combined with joint pain — seek urgent care, as this may indicate infection
What to Expect at Your Appointment
Your doctor or hand specialist will typically:
- Take a history — asking about your symptoms, when they started, what makes them better or worse, and your hand use
- Examine your hand — feeling the joint, testing range of motion, checking grip and pinch strength, and performing specific tests like the Grind Test (pressing and rotating the thumb into the base to check for pain and grinding)
- Order X-rays — a standard hand X-ray or a specialized Robert view can show joint narrowing, bone spurs, and the stage of arthritis
- Make a diagnosis — based on the combination of your symptoms, examination findings, and imaging
For a detailed explanation of diagnostic tests and staging, visit our diagnosis and imaging guide.
What Comes Next
Once you have a diagnosis, treatment depends on the cause and severity. For rhizarthrosis, the approach is usually step-by-step:
- Mild symptoms: Splinting, hand exercises, and activity modification — see our conservative treatment guide
- Moderate symptoms: Cortisone injections, hand therapy, and possibly a custom splint — learn about choosing the right splint
- Severe or advanced arthritis: Surgical options including trapeziectomy or joint replacement — explore our surgical treatment guide
The most important step is getting an accurate diagnosis. Many patients live with unnecessary pain because they assume it is just part of aging. Effective treatments exist at every stage of thumb arthritis, and earlier treatment often leads to better outcomes.
Medical Disclaimer
This article was prepared by the Hand Health Medical Advisory Board for educational purposes only. It is based on current medical literature and clinical guidelines, but it does not replace professional medical advice. Every patient’s situation is unique. Please consult your doctor or hand specialist before making any decisions about your treatment. If you are experiencing severe or worsening symptoms, seek medical attention promptly.
With your diagnosis clear, explore all non-surgical treatment options backed by clinical evidence.
Non-Surgical Treatments