Key Takeaways
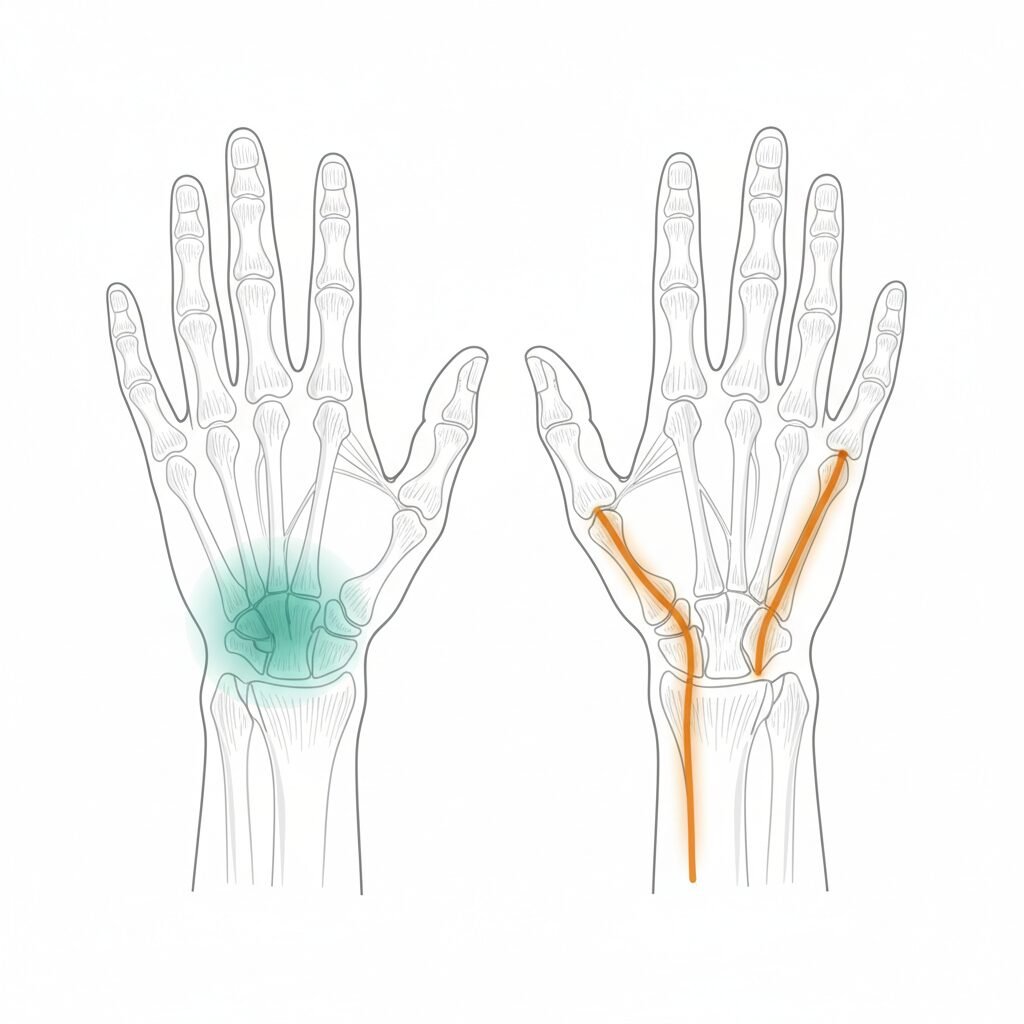
- Rhizarthrosis is joint wear (arthritis) at the thumb base; de Quervain’s is tendon inflammation on the thumb side of the wrist.
- The location of pain is the biggest clue: deep in the joint for arthritis, over the wrist tendons for de Quervain’s.
- Doctors use different hands-on tests — the Grind Test for arthritis and the Finkelstein Test for de Quervain’s.
- It is possible to have both conditions at the same time, especially in women over 50.
- Treatments differ significantly, so getting the right diagnosis matters.
When your thumb hurts near the wrist, it can be confusing to figure out what is going on. Two of the most common culprits — rhizarthrosis (thumb arthritis) and de Quervain’s tenosynovitis — cause pain in a similar area but are very different conditions. Getting the right diagnosis is important because the treatments are not the same.
At a Glance: Rhizarthrosis vs De Quervain’s
Here is a side-by-side comparison to help you understand the key differences:
| Feature | Rhizarthrosis (Thumb Arthritis) | De Quervain’s Tenosynovitis |
|---|---|---|
| What it is | Cartilage wear in the CMC joint | Inflammation of thumb-side wrist tendons |
| Where it hurts | Deep at the base of the thumb, in the fleshy mound | Over the wrist tendons, thumb side of wrist |
| Pain triggers | Pinching, gripping, opening jars | Wrist movements, lifting, wringing |
| Who gets it | Mostly women over 50; increases with age | Women 30-50, new parents, repetitive wrist use |
| Onset | Gradual, over months to years | Often sudden or over days to weeks |
| Grinding sensation | Yes (crepitus) | No (may feel squeaking) |
| Morning stiffness | Yes, usually less than 30 minutes | Minimal |
| Visible changes | Bony bump, squared-off thumb base | Swelling along the wrist tendons |
| Diagnostic test | Grind Test (CMC compression) | Finkelstein Test |
| X-ray findings | Joint narrowing, bone spurs | Normal (soft tissue problem) |
Understanding Each Condition
Rhizarthrosis: A Joint Problem
Rhizarthrosis is osteoarthritis of the first carpometacarpal (CMC) joint — the saddle-shaped joint where the thumb metacarpal bone sits on the trapezium bone. Over time, the cartilage lining this joint wears thin, leading to friction, inflammation, and eventually bone-on-bone contact.
This condition develops gradually. Patients typically notice increasing pain with pinching and gripping activities. Opening jars, turning keys, and writing become progressively harder. The joint itself may enlarge and develop a squared-off appearance. Research shows that 25-33% of postmenopausal women have radiographic evidence of CMC arthritis, making it one of the most common forms of hand osteoarthritis.
For a complete overview, see our guide to thumb joint anatomy and our article on CMC arthritis stages.
De Quervain’s: A Tendon Problem
De Quervain’s tenosynovitis involves inflammation of two tendons that run through a tunnel (the first dorsal compartment) on the thumb side of the wrist: the abductor pollicis longus and the extensor pollicis brevis. When the tunnel becomes irritated or thickened, the tendons cannot glide smoothly, causing pain with wrist and thumb movement.
This condition often has a more sudden onset, frequently linked to repetitive wrist movements, a new activity, or hormonal changes (it is common during pregnancy and the postpartum period). The pain tends to be sharper and more on the surface than the deep ache of arthritis.
The Diagnostic Tests Your Doctor Will Use
The Grind Test (for Rhizarthrosis)
Your doctor grasps your thumb and pushes it firmly into the base while rotating it in a circular motion. This compresses the CMC joint surfaces together. If this reproduces your typical deep pain and you feel a grinding or crunching sensation, the test is considered positive for arthritis. Studies show the Grind Test has a sensitivity of about 42-53% and specificity of 80-93% for CMC arthritis — meaning a positive test is quite reliable, but a negative test does not rule it out.
The Finkelstein Test (for De Quervain’s)
You tuck your thumb inside a closed fist, then bend your wrist toward your little finger. This stretches the inflamed tendons in the first dorsal compartment. If this produces a sharp, sometimes intense pain over the thumb-side wrist tendons, the test is positive for de Quervain’s. This test is very sensitive — it catches most cases — but can occasionally be positive in other conditions too.
Can You Have Both at the Same Time?
Yes, and this is more common than many patients realize. Studies suggest that co-existing CMC arthritis and de Quervain’s occurs in approximately 10-15% of patients presenting with thumb-side wrist pain, particularly in women over 50. When both conditions are present, treatment needs to address each one.
Signs that both may be present:
- You have pain both deep in the thumb base (joint) and along the wrist tendons
- Both the Grind Test and Finkelstein Test are positive
- X-rays show joint changes but your pain pattern does not match arthritis alone
- A cortisone injection into the CMC joint helps only partially
How Treatments Differ
For Rhizarthrosis
- Splinting: A CMC-stabilizing thumb splint to protect the joint — see our splint guide
- Hand therapy: Strengthening the muscles around the joint to improve stability
- Cortisone injections: Into the CMC joint for 3-6 months of relief
- Surgery (if conservative treatment fails): Trapeziectomy or joint replacement — explore options in our surgical treatment guide
For De Quervain’s
- Rest and activity modification: Avoiding the triggering movements
- Thumb spica splint: Immobilizing the wrist and thumb to rest the tendons
- Anti-inflammatory medications: NSAIDs to reduce tendon inflammation
- Cortisone injection: Into the tendon sheath (not the joint) — effective in about 80% of cases
- Surgery (rare): Release of the first dorsal compartment if injections fail
When to See Your Doctor
See a doctor or hand specialist if:
- Your thumb or wrist pain has persisted for more than 2-3 weeks
- Pain is interfering with your daily activities or work
- Over-the-counter treatments are not providing relief
- You are unsure which condition you have — an accurate diagnosis guides the right treatment
Getting the correct diagnosis is especially important because the injection techniques are different (joint vs. tendon sheath), and an injection in the wrong location will not help. A hand specialist can usually distinguish between the two conditions with a careful examination and standard X-rays.
For more information on the diagnostic process, see our diagnosis and imaging guide, or start with our comprehensive start here page.
Medical Disclaimer
This article was prepared by the Hand Health Medical Advisory Board for educational purposes only. It is based on current medical literature and clinical guidelines, but it does not replace professional medical advice. Every patient’s situation is unique. Please consult your doctor or hand specialist before making any decisions about your treatment. If you are experiencing severe or worsening symptoms, seek medical attention promptly.
With your diagnosis clear, explore all non-surgical treatment options backed by clinical evidence.
Non-Surgical Treatments