Key Takeaways
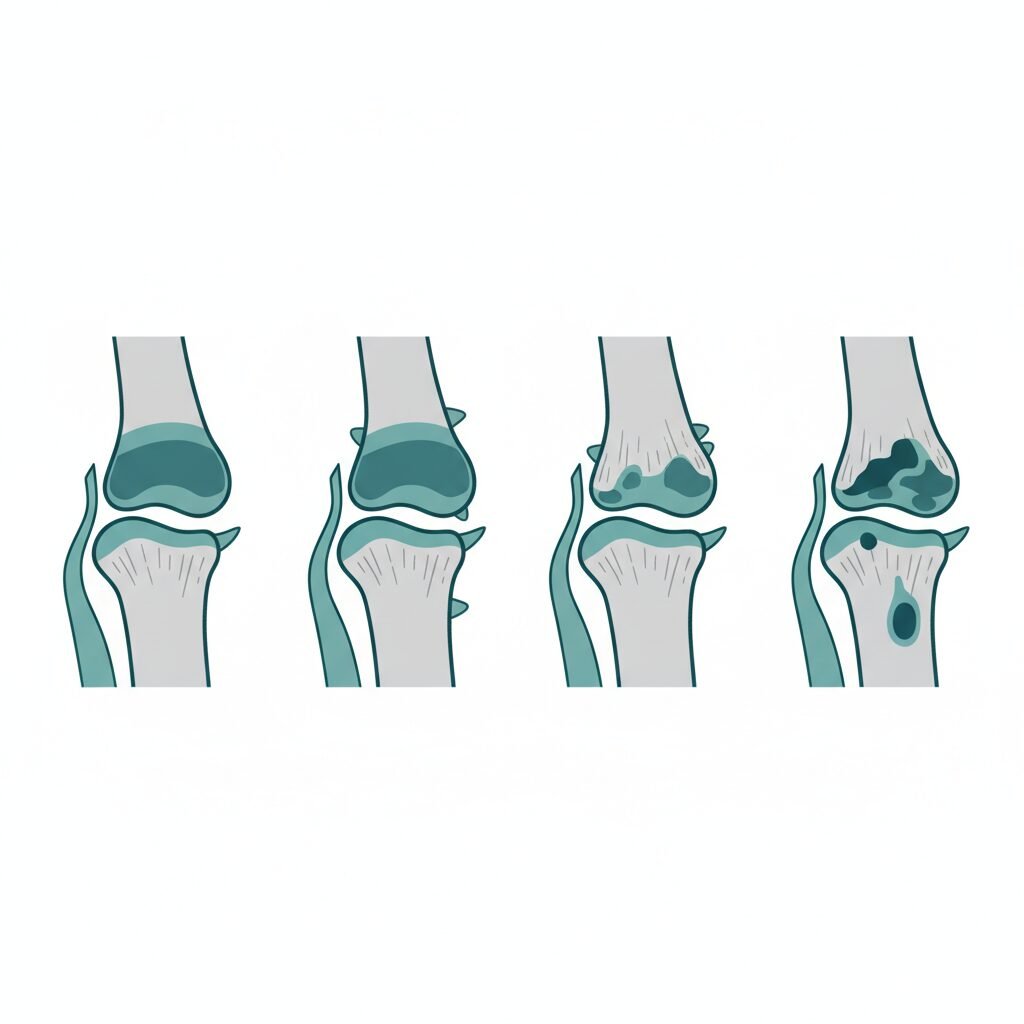
- CMC joint arthritis (rhizarthrosis) is classified into 4 Eaton stages based on X-ray findings, from early (stage I) to advanced (stage IV).
- Your X-ray stage does not always match your pain level — some people with advanced X-ray changes have mild symptoms, and vice versa.
- Treatment is matched to your stage, starting with conservative options in stages I-II and considering surgery in stages III-IV when conservative measures fail.
- Understanding your stage helps you make informed decisions and set realistic expectations for treatment.
If your doctor has mentioned “Eaton stage” or “CMC arthritis staging” during your visit, you are probably wondering what it means for your treatment. The Eaton-Littler classification is the system doctors use worldwide to describe how far your thumb arthritis has progressed. Understanding where you fall on this scale can help you make sense of your diagnosis and know what comes next.
What Is the CMC Joint?
The carpometacarpal (CMC) joint is the saddle-shaped joint where the thumb metacarpal bone sits on the trapezium bone, right at the base of your thumb. It is one of the most mobile joints in the hand, allowing your thumb to oppose (touch) each fingertip — the movement that makes the human hand uniquely capable. But this remarkable mobility comes at a cost: the joint is inherently unstable and vulnerable to wear.
For a detailed look at the anatomy, visit our anatomy and biomechanics guide.
The 4 Eaton Stages Explained
Stage I: Pre-Arthritis
What the X-ray shows: The joint looks nearly normal. The joint space may appear slightly widened due to fluid or ligament laxity. There are no bone spurs (osteophytes) and no visible cartilage loss.
What you may feel:
- Occasional aching at the thumb base after heavy use
- A sense of the thumb feeling “loose” or unstable
- Pain may come and go, often dismissed as normal
- Grip and pinch strength are usually normal
Recommended treatment:
- Activity modification — avoid or adapt activities that trigger pain
- Thumb splint during aggravating activities — see our splint guide
- Hand exercises to strengthen the stabilizing muscles — see our exercise guide
- Anti-inflammatory medications as needed
- In some cases, ligament reconstruction may be considered to prevent progression
Stage II: Early Arthritis
What the X-ray shows: Slight narrowing of the joint space (cartilage beginning to thin). Small bone spurs (osteophytes less than 2mm) start appearing at the joint margins. Possible slight subluxation (shifting) of the joint.
What you may feel:
- More consistent pain with pinching and gripping
- Morning stiffness lasting 10-20 minutes
- A grinding sensation (crepitus) when moving the thumb
- Mild reduction in pinch strength
- Possible slight swelling at the thumb base
Recommended treatment:
- All Stage I measures plus:
- More consistent splint use, including a custom-made orthosis
- Formal hand therapy program
- Cortisone injection if pain is not controlled by other measures — typically provides 3-6 months relief
- Consideration of hyaluronic acid or PRP injections — see our injection comparison article
Stage III: Established Arthritis
What the X-ray shows: Significant joint space narrowing (most of the cartilage is gone). Large bone spurs (osteophytes greater than 2mm). Subluxation of the metacarpal on the trapezium (the thumb bone is visibly shifting). Subchondral sclerosis (hardened bone beneath the missing cartilage). The STT (scaphotrapeziotrapezoidal) joint next door still looks normal.
What you may feel:
- Daily pain that limits common tasks — opening jars, writing, using keys
- Noticeable loss of grip and pinch strength
- Visible bony enlargement at the thumb base
- Possible Z-deformity of the thumb (thumb appears zigzagged)
- Reduced range of motion
- Pain may now occur at rest or at night
Recommended treatment:
- Continue conservative measures (they can still help with symptoms)
- Surgery should be discussed if conservative treatment has been tried for 3-6 months without adequate relief
- Surgical options: trapeziectomy (with or without ligament reconstruction) or joint replacement
- See our comparison of trapeziectomy vs joint replacement
Stage IV: Advanced (Pantrapezial) Arthritis
What the X-ray shows: Everything in Stage III plus involvement of the STT joint (the joint next to the CMC). This means arthritis has spread beyond the thumb base to involve the trapezium’s other joint surfaces. Large osteophytes, significant subluxation, and possibly cyst formation in the bone.
What you may feel:
- Significant daily pain and functional limitation
- Substantial loss of grip and pinch strength
- Marked thumb deformity and stiffness
- Pain with almost any thumb use
- Impact on quality of life and independence
Recommended treatment:
- Surgery is usually recommended at this stage
- Trapeziectomy (complete trapezium removal) is the most common procedure because the entire bone is involved
- Joint replacement is generally less suitable because the adjacent joint is also affected
- Arthrodesis (joint fusion) may be considered in younger, very active patients
- For surgical details, visit our surgical treatment guide
Your X-Ray Does Not Tell the Whole Story
This is one of the most important things to understand about CMC arthritis staging: there is often a mismatch between what the X-ray shows and how much pain you feel.
Research consistently demonstrates this pattern:
- Some patients with Stage III X-rays have relatively mild symptoms and manage well with conservative treatment
- Some patients with Stage I-II X-rays have significant pain that limits daily life
- Studies show only a moderate correlation (about 50-60%) between radiographic severity and patient-reported pain and disability
What this means for you: treatment decisions should be based primarily on your symptoms, function, and quality of life — not solely on what the X-ray shows. A doctor who says “your X-ray looks bad, so you need surgery” without considering how you are actually doing may be oversimplifying. Conversely, if you are in significant pain and someone dismisses it because your X-ray looks mild, seek a second opinion.
What Stage Am I?
Only your doctor can determine your Eaton stage based on proper X-rays (ideally a Robert view of the thumb). However, the symptom descriptions above can give you a general sense of where you might fall. Bring this knowledge to your next appointment and ask:
- “What Eaton stage is my arthritis?”
- “Are the adjacent joints involved, or is it just the CMC joint?”
- “Based on my symptoms and stage, what treatments do you recommend trying first?”
For more on the diagnostic process, see our diagnosis and imaging guide. For a comprehensive view of treatment options at every stage, explore our treatment comparison page and start here page.
Medical Disclaimer
This article was prepared by the Hand Health Medical Advisory Board for educational purposes only. It is based on current medical literature and clinical guidelines, but it does not replace professional medical advice. Every patient’s situation is unique. Please consult your doctor or hand specialist before making any decisions about your treatment. If you are experiencing severe or worsening symptoms, seek medical attention promptly.
Now that you understand the anatomy, learn how rhizarthrosis is diagnosed and what the Eaton stages mean.
Diagnosis Guide