Key Takeaways
- Cortisone injections provide significant pain relief for about 70% of patients with thumb arthritis, typically lasting 3-6 months.
- The procedure takes only a few minutes and most patients describe it as a brief, moderate discomfort rather than severe pain.
- Most doctors recommend no more than 2-3 injections per year to avoid potential cartilage damage.
- Injections work best as part of a combined approach with splinting and hand therapy, not as a standalone treatment.
When splinting and therapy are not providing enough relief for your thumb arthritis, your doctor may recommend a cortisone injection. It is one of the most common treatments for rhizarthrosis, and for many patients it provides meaningful relief that can last for months. Here is what you need to know — from the science behind it to what the injection actually feels like.
How Cortisone Injections Work
Cortisone (corticosteroid) is a powerful anti-inflammatory medication. When injected directly into the CMC joint, it reduces the inflammation that causes pain, swelling, and stiffness. Unlike oral anti-inflammatory drugs that affect your whole body, an injection delivers a concentrated dose right where it is needed.
The injection typically contains two components:
- A corticosteroid (such as triamcinolone or methylprednisolone) — the anti-inflammatory medication
- A local anesthetic (such as lidocaine) — provides immediate but temporary pain relief and confirms the injection is in the right spot
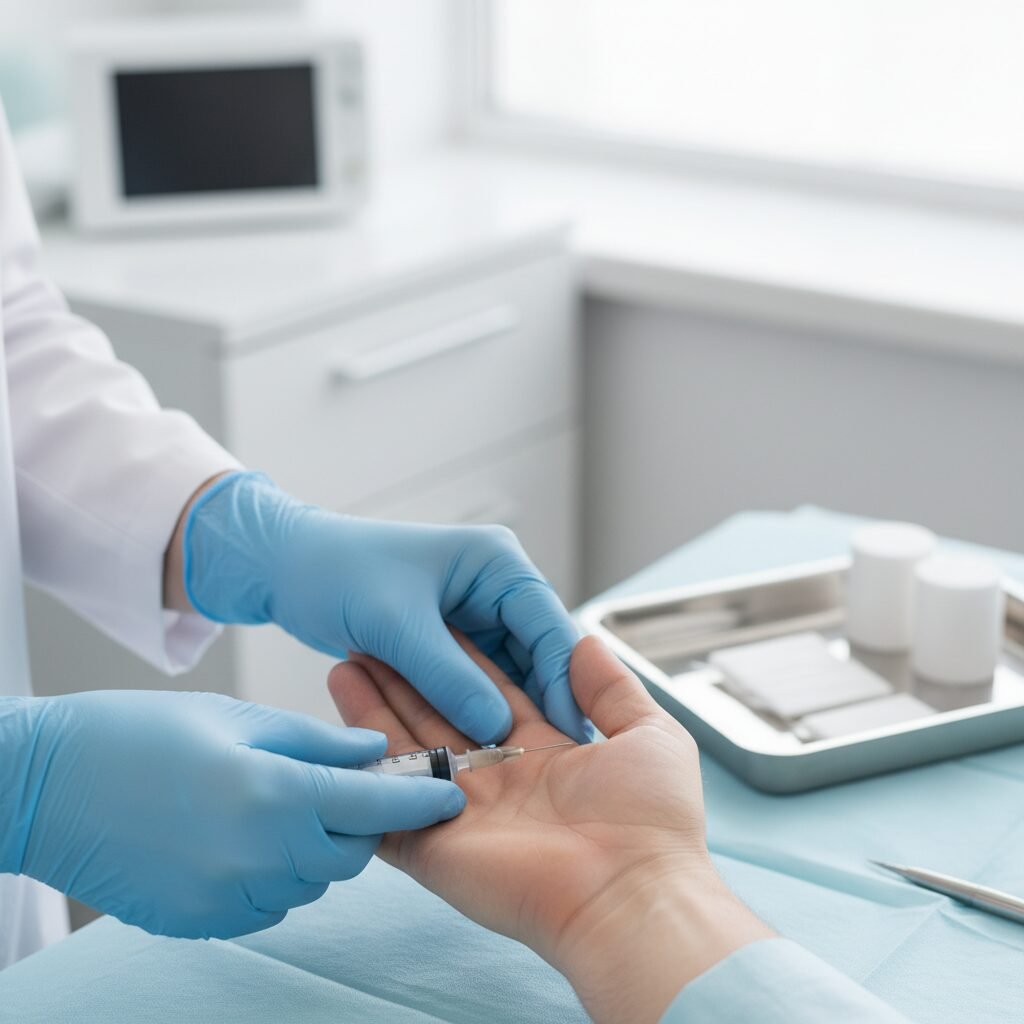
What Happens During the Procedure
The injection is typically performed in your doctor’s office and takes about 5-10 minutes total:
- Positioning: Your hand is placed palm-down on a table. The doctor locates the CMC joint by feeling the bones at the base of your thumb.
- Cleaning: The skin is cleaned with an antiseptic solution.
- Optional numbing: Some doctors apply a cold spray or topical anesthetic before the injection.
- Injection: A thin needle is inserted into the joint space. You may feel pressure and a brief sting. The medication is injected slowly.
- Aftercare: A small bandage is applied. You can usually drive home and resume light activities the same day.
Some doctors use ultrasound guidance to ensure the needle is precisely in the joint. Research shows ultrasound-guided injections have higher accuracy rates (95% vs. 75% for landmark-guided), which may improve outcomes.
How Much Does It Hurt?
This is the question most patients want answered first. Honestly, it varies from person to person, but most patients describe it as:
- A brief sharp sting when the needle enters the skin (1-2 seconds)
- A sensation of pressure or fullness as the medication enters the joint
- Overall, uncomfortable but tolerable — most rate it 3-5 out of 10 on a pain scale
- The local anesthetic starts working within seconds, and many patients feel immediate relief
A common experience: the first 24-48 hours after injection may actually be more painful than before (called a “cortisone flare”) as the body reacts to the medication crystals. This is normal and resolves on its own. Ice and over-the-counter pain medication can help during this period.
How Long Does the Relief Last?
Clinical studies show the following pattern:
- Immediate relief (first few hours) — from the local anesthetic; this wears off
- Full cortisone effect — typically kicks in after 3-7 days
- Peak benefit — usually at 2-4 weeks
- Duration of relief — 3-6 months on average, though this varies widely
Some patients get 6-12 months of relief, while others notice the effect fading after 6-8 weeks. Research suggests the first injection tends to provide the longest relief, with subsequent injections sometimes being less effective. A 2015 meta-analysis found that about 70% of patients experience meaningful pain reduction after a CMC joint cortisone injection.
Risks and Side Effects
Cortisone injections are generally safe, but like any medical procedure, they carry some risks:
- Post-injection flare (common, 10-25%) — temporary increased pain for 24-48 hours
- Skin thinning or discoloration (uncommon) — at the injection site, more common with repeated injections
- Infection (rare, less than 1 in 10,000) — watch for increasing redness, warmth, and fever
- Tendon weakening (rare) — a concern if the injection goes into a tendon rather than the joint
- Temporary blood sugar elevation — important for patients with diabetes; discuss with your doctor
- Cartilage effects — repeated injections (more than 3-4 per year) may accelerate cartilage breakdown; this is why most doctors limit the number
How Many Can You Have?
There is no absolute rule, but most hand specialists follow these guidelines:
- No more than 2-3 injections per year in the same joint
- At least 3-4 months between injections
- If 2-3 injections provide diminishing relief, it may be time to discuss other options
- There is no strict lifetime limit, but the joint should be reassessed if injections stop working
An injection that provides good relief for several months is a positive sign — it confirms the pain is coming from the CMC joint and buys time while you pursue other treatments like hand therapy and splinting.
Alternatives to Cortisone
If cortisone injections are not suitable for you or have stopped working, other injection options exist:
- Hyaluronic acid injections — may provide similar relief with fewer side effects; see our article on PRP and hyaluronic acid injections
- PRP (platelet-rich plasma) — emerging evidence for longer-lasting effects
- Surgical options — when all conservative treatments have been exhausted; learn more in our surgical treatment guide
For a comprehensive overview of all non-surgical treatments, visit our conservative treatment guide. To compare treatment approaches at different stages of disease, see our treatment comparison page.
Medical Disclaimer
This article was prepared by the Hand Health Medical Advisory Board for educational purposes only. It is based on current medical literature and clinical guidelines, but it does not replace professional medical advice. Every patient’s situation is unique. Please consult your doctor or hand specialist before making any decisions about your treatment. If you are experiencing severe or worsening symptoms, seek medical attention promptly.
Compare every treatment option side by side before making any decisions.
Treatment Comparison